Spinal Seating Modules
Wheelchair seating – A complex puzzle
Wheelchair seating can be very complicated due to the way in which seating components interact with each other, and affect the client’s posture, pressure, function and comfort.
Having completed a seating assessment the clinician may have a large amount of information regarding the client’s needs, vulnerabilities and capabilities. The clinician may need to summarise and prioritise the identified issues, needs and goals with the client for the desirable outcomes of the seating intervention. This module aims to provide a problem solving framework for seating intervention and wheelchair prescription.
A Problem Solving Framework for Seating Intervention and Wheelchair Prescription
- Keep the big picture in mind
- Be systematic in identifying seating issues – Size, Shape and Functions
- Recognise key relationships between the client and the wheelchair
- Formulate trials to explore different configurations to see if they produce stable outcomes
- Work as a team: share information and ideas with the client and other therapists
- Persevere!!
Keep the big picture in mind
The four interrelated goals in seating are pressure management, posture support, functional capability, and client comfort. They help to keep the big picture in mind. Modules 2 to Module 5 assist clinicians to individualise the four overarching goals specific to each client.
It is important to recognise that a simple adjustment or alteration to a seating component may result in other components also needing to be adjusted - a domino effect on the client’s seating needs or goals. For example, trialling an alternative pressure care cushion with a different profile or thickness may require height adjustments to the headrest, back support, armrests and footplates in order to maintain client’s level of pressure care, postural support, functional capacity and comfort. Like a puzzle, each piece is linked together to form the big picture.
For each possible intervention, the clinician needs to step back and consider the impact it has on the four interrelated goals, and to discuss with the client. In cases where the optimisation of one seating goal conflicts with another, an appropriate compromise or trade-offs may be necessary to establish the agreed seating intervention plans.
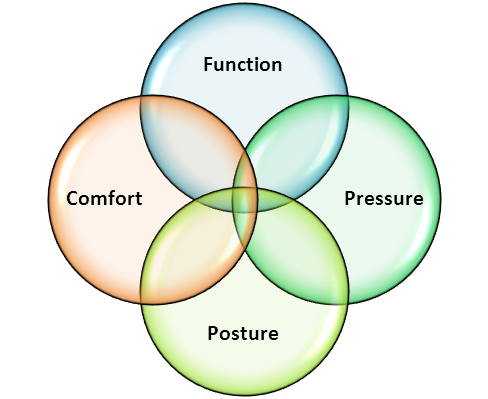
The four goals of spinal seating
Case scenario:
A client with a T3 spinal cord injury has a moderate fixed mid thoracic kyphosis. His manual wheelchair is fitted with a tall rigid backrest but he has a tendency to lose his balance forward. Some possible intervention options may be:
- To move his pelvis forward on the seat to gain trunk stability
- To adjust the backrest angle to be more recline
- To try a tension upholstery backrest
- To use a chest harness
For each options above, consider:
- What consequences are likely have on the client in terms of pressure, posture, function and comfort?
- How each option would affect the configuration of the wheelchair, such as the stability of the wheelchair and wheel propulsion effort?
After considering all the consequences, which option might address the client’s issue while meeting his pressure care needs, postural stability, functional requirements and comfort?
3. Be systematic
Taking a systematic approach can be helpful in managing all the information involved.
Using the seating assessment forms, summarise the key findings and issues so they can be easily referred to throughout the seating intervention.
- Module 2: Initial Interview form
- Module 3: Basic MAT form
- Module 4: Body measurement form
- Module 5 :PWC Specification Form and
- Module 5: MWC Specification Form
To identify key problems and requirements that have been reported or observed, consider ‘size’, ‘shape’ and ‘function’ are useful intervention strategies for identifying issues and choosing equipment appropriate to the client’s needs. These will determine potential seating interventions.
- Size: does the size of the wheelchair and the seating system (Module 5) accommodate the body measurements requirements (Module 4) to provide suitable support and enable function?
- Shape: does the wheelchair and seating system shape (Module 5) accommodate the client’s body shape and range of motions to provide postural support and balance requirements (Module 3)? Does it allow for a comfortable and supported seating arrangement?
- Function: does the seating and mobility systems (Module 5) are intended to enable the client to function in all life roles and to access their environment and community (Module 2)?
The seating and mobility system needs to fit the client with regard to ‘size’, ‘shape’ and ‘function’.
4. Recognise key relationships between the client and the wheelchair
The wheelchair should be considered as both as a seating system (considering the interactions between the wheelchair and the user) and as a mobility system (considering the interactions between the chair and the environment).
As a seating system the primary consideration is how the wheelchair interacts with the client’s body. Module 7 (Postural interventions) and Module 8 (Pressure Management) will provide key intervention strategies to meet these seating goals.
As a mobility system, the wheelchair should optimise the client’s level of functional mobility and match the client’s need for access into the environment and community. Module 9 (Manual wheelchairs and propulsion-assist devices) and Module 10 (Power wheelchairs) will provide key intervention strategies to prescribe and optimise mobility system.
5. Formulate trials
Trials are a critical process in a seating intervention. A trial reveals potential problems in the seating and mobility systems, which must work together to allow the client to interact with their environment while remaining adequately supported. The trial should include the client performing daily activities in appropriate environments which may reveal considerations that are not apparent in the clinic space.
Providing adequate education on equipment operation and care instruction to the user and carer should be considered an essential part of the trial process. It may be useful to document the client’s feedback and trial outcomes specific to the goals set in a table fomat.
The outcome of the trial may be misleading if the wheelchair was not used or configured correctly. Clients should understand how the design features of the trial equipment relate to their needs and goals as this will help promote collaboration and stimulate effective feedback post-trial.
It is prudent to record dimensions of a seating configuration prior to making any changes to create a reference for comparison with other configurations.
In progressive trials, where different equipment is being trialled for comparison, be aware that changing one component can require significant reconfiguration of the chair to create the same effective setup.
Examples
In a manual chair, changing from a rigid backrest to an upholstery backrest often results in a change of effective seat depth and wheelchair stability that should be corrected in order to evaluate a valid comparison.
Similarly, when trialling different cushion types, be aware of the effective height that that cushion has, as backrests, leg hangers and arm supports may need to be adjusted to accommodate any difference.
Problems can arise when the equipment that has been scripted differs from the equipment which was trialled. While there may be occasions where the preferred size or configuration of equipment is unavailable for trial, the closer the trial equipment is to that being scripted the less scope there is for an adverse outcome.
5. Work as a team
With the client’s permission, communicate with, or refer to other relevant health professionals, rehabilitation engineers and equipment suppliers who assist in meeting the established goals.
It may be important to involve the client’s family/carers in trialling new wheelchair or seating setup, especially, if they are providing assistance to the client in transfer, repositioning in wheelchair, operation and maintenance of new equipment. They can also provide feedback the outcomes of seating trials and monitor skin status.
6. Persevere!!
Even with careful planning there may be unexpected issues that only become apparent with a proper trial. Do not become disheartened! Each trial provides more information to help understand the limitations and requirements of the client’s seating and mobility needs. To gain the most out of each trial it is helpful to monitor and evaluate the outcome of seating interventions that have been tried. Ask the client to record what worked well and what did not. A record of usage (when, where and for how long) may also be useful in clarifying the typical environment of use.
Fine tuning of the seating configuration of a trial setup or across multiple trials may be required to obtain the best outcome to meet a client’s clinical needs and personal preferences. A small adjustment can often make the difference between a setup that works and a setup that does not. Where possible, adjusting a single component at a time can help to establish whether there is a direct relationship between the cause and effect for a seating outcome.
If you have reached the limit of available options you can refer to a Spinal Seating Service for advice or a consultation to explore complex seating solutions or custom fabricated seating solutions.