Justice Health and Forensic Mental Health Network (the Network) identified inconsistent metabolic monitoring as a patient safety risk, and resourced a project team to address this issue.
Patients prescribed psychotropic medications are at increased risk of physical health side effects such as metabolic syndrome. These risks can be identified through regular physical health checks, referred to as metabolic monitoring.
View a poster from the Centre for Healthcare Redesign graduation, December 2019.
Aim
We aim to increase:
- the number of patients with a metabolic monitoring electronic health record (PAS) alert from 24.9% to 50% by December 2019
- the number of patients with a metabolic monitoring waitlist from 0% to 50% by June 2020
- the number of patients with a metabolic monitoring assessment in the electronic health record (JHeHS) from 4.4% to 50% by December 2020.
This will achieve our goal of improving metabolic monitoring services for patients prescribed psychotropic medications.
Note: Data was not able to be sourced for past metabolic monitoring waitlists as waitlist are removed once it is transferred to an arrived appointment.
Benefits
- Establish a process to identify patients prescribed psychotropic medications
- Reduce the risk of adverse health events to patients prescribed psychotropic medications through metabolic monitoring
- Increased provision of person-centred care to patients prescribed psychotropic medication
- Increased staff satisfaction with clear guidance and clarity surrounding roles and responsibilities of metabolic monitoring
- Cost efficiencies and improved use of resources through early prevention, detection, and intervention of metabolic syndrome.
Background
Psychotropic medications are used to treat symptoms of mental illness and play an important role in a patient’s treatment plan. However, the adverse side effects of psychotropic medications are common and potentially serious requiring patients to be metabolically monitored.
In 2017 a coroner’s investigation found that the prescribing of concurrent psychotropic medications and the lack of metabolic monitoring contributed to a patient’s death.
In 2018, an internal metabolic monitoring audit was conducted to assess compliance to the network’s metabolic monitoring guidelines. The Network was given recommendations to improve compliance.
During the diagnostics stage of this clinical redesign project, it was identified that 63% of Network patients prescribed medications, are on one or more psychotropic medications.
Implementation
Solution 1: Fit for purpose JHeHS form
Our first solution is to create a fit for purpose metabolic monitoring JHeHS form. A new form has been drafted based on the feedback received during our solutions workshops. The form has been approved for development and we are working with information and communications technology and information management departments to progress the build.
Solution 2: Standardised handover script
Our second solution is to create a standardised handover script to identify patients on psychotropic medications. A script has been created using the Introduction Situation Background Assessment Recommendation (ISBAR) tool with medical and nursing staff. The script is currently being evaluated using the PDSA (plan, do, stop, act) cycle.
Solution 3: Dedicated metabolic monitoring clinic
Our third solution is to set up a dedicated metabolic monitoring clinic that is a one stop shop to complete a comprehensive assessment. This involved the creation of a new psychotropic medication – metabolic monitoring Patient Administration System (PAS) alert to identify patients. In addition, PAS Metabolic Monitoring clinics were created to wait list patients for appointments. This solution is being piloted in four correctional sites for 12 weeks, this includes the monitoring of clinic processes for efficiency, PAS and JHeHS data collection, patient surveys and staff surveys.
Solution 4: Review of ECG results
Our fourth solution is to review the process of ECG results review and signed off. A working group is in the process of reviewing options for ECG results and this includes outsourcing.
In addition, the above solutions are informing the review of the current psychotropic guidelines currently underway.
Status
Implementation - The initiative is ready for implementation, is currently being implemented, piloted or tested.
Dates
January – December 2019
Implementation sites
- Metropolitan Special Programs Centre 3, Long Bay Complex
- Silverwater Women’s Correctional Centre
- Shortland 3/4 Correctional Centre
- Cobham Youth Justice Centre
Partnerships
Centre for Healthcare Redesign
Results
This data has been collected from the four implementation sites of the metabolic monitoring nurse led clinic pilot. Data was measured on a weekly basis, and included the number of patients with metabolic monitoring PAS Alerts, waitlists and arrived appointments.
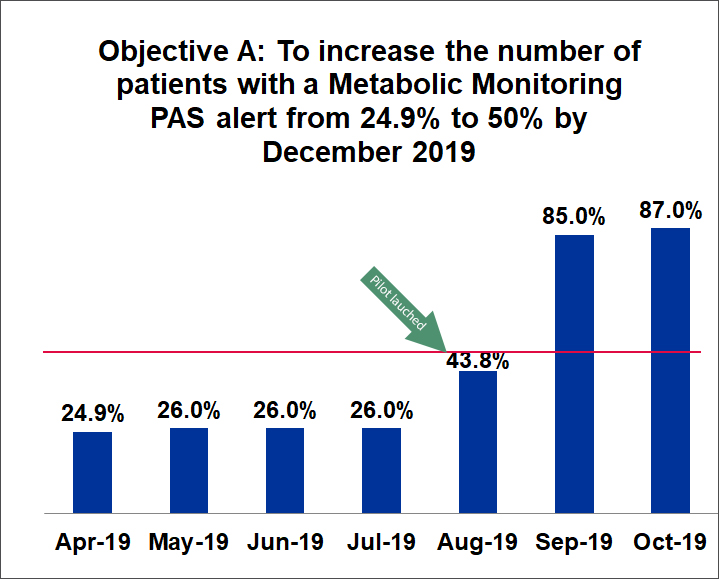
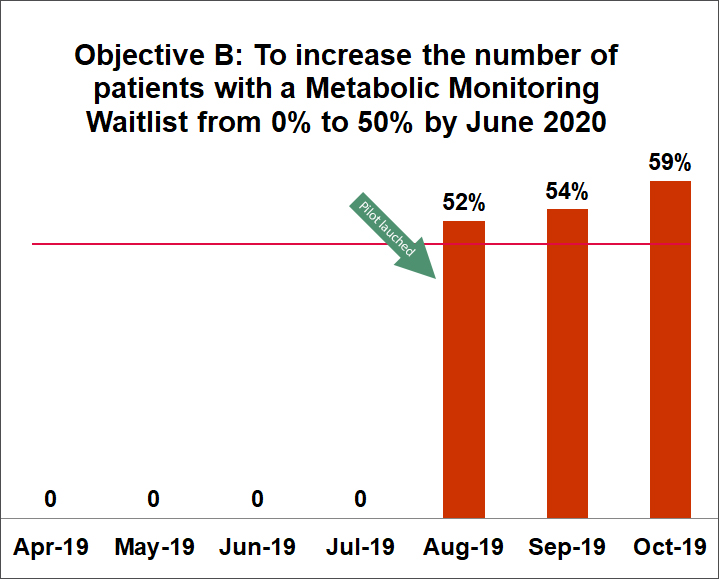
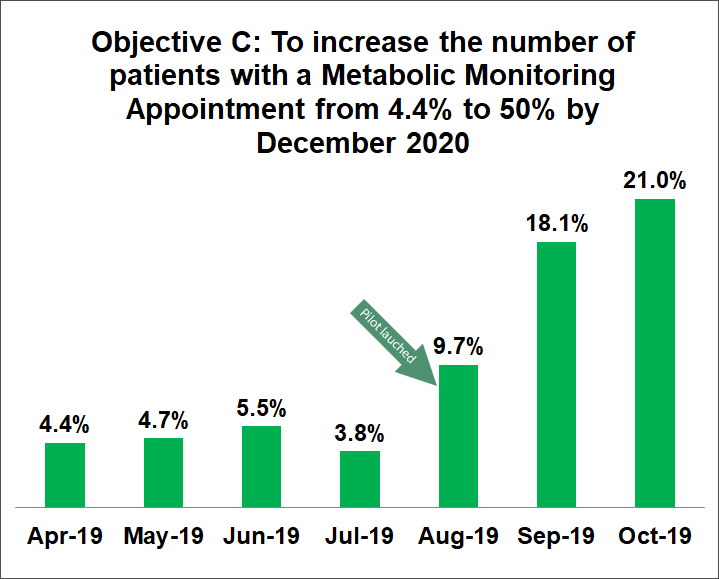
(Objective B: Data was not able to be sourced for past metabolic monitoring waitlists, as waitlist are removed once it is transferred to an arrived appointment.)
Lessons learnt
- Acknowledging the importance in understanding the culture and climate of the environment where the change is occurring. In particular, the impact change creates on different professional groups.
- Remembering that change does not occur in isolation, and being able to foresee and manage the ripple effect that can occur with a singular change. A constant challenge was working within other team’s timeframes and priorities, when working to the projects tight timeframes.
Contact
Allison Preobrajensky
Performance Integration Manager
Clinical Business Unit
Justice Health and Forensic Mental Health Network
Phone: 02 9700 3026
Allison.preobrajensky@health.nsw.gov.au
