Bone health
This fact sheet is for people who have had a blood and marrow transplant (BMT).
BMT patients may experience health complications in the months or years following the transplant. Long-term follow up has an important role in the early detection of any health issues.
This fact sheet has general information about ways to look after your health. If you have specific concerns, speak to your BMT team or your doctor for further information and advice.
What are the issues that could affect my bone health?
After illness or treatment, some people develop a health condition that affects their bones. This may be caused by cancer treatments, such as radiation, chemotherapy and steroid use.
Bone conditions
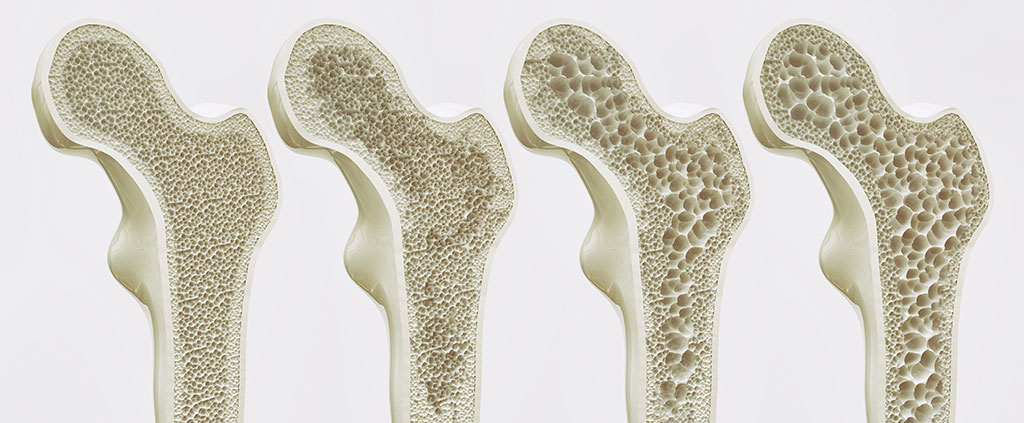
- Osteopenia – bone mass is reduced, increasing the risk of osteoporosis.
- Osteoporosis – there is further bone loss and a high risk of bone fractures.
- Avascular necrosis – the blood supply to the bones is damaged, causing the bones to break down faster than the body can rebuild them.
What are the symptoms?
Unfortunately, there are no symptoms of osteopenia. You may not know that you have osteopenia until you break a bone after having a minor trip or fall.
Symptoms of osteoporosis may include back pain, a reduction in height over time, a stooped posture and a bone fracture that occurs more easily than expected. Tooth loss can also be a symptom.
Avascular necrosis has limited symptoms of in the early stages. As avascular necrosis progresses, you may experience joint pain.
How are these issues diagnosed?
- Osteopenia and osteoporosis – bone density scan or test.
- Avascular necrosis – an x-ray, magnetic resonance imaging (MRI), computerised tomography (CT) or bone scan.
How are bone health issues treated?
- Osteopenia and osteoporosis – calcium and vitamin D are prescribed. However, if your bone marrow density has decreased significantly, you may be prescribed specific medication to reduce bone loss and increase your bone density. These drugs include bisphosphonates (biz-fos-fo-nate), such as alendronate and zoledronic acid and antibody treatments, such as denosumab.
- Avascular necrosis – conservative (non-surgical) treatment with bone strengthening medications, pain relief medicines and rest may be recommended, but in most cases joint surgery or replacement is required.
How can I look after my bones?
There are things you can do to look after your bone health.
- Bone assessments – during your long-term follow-up appointment, your doctor can check your hormonal and vitamin D levels (using a blood test). You may do a dual-energy x-ray absorptiometry (DXA) scan to check your bone density.
- Don’t smoke – your general practitioner (GP) can support you to reduce or quit smoking.
- Reduce alcohol consumption – drink in moderation only.
- Maintain a healthy diet – calcium is vital for building and maintaining healthy bones. It is found in a nutritious diet that includes dairy foods, fish (salmon or sardines) and dark green leafy vegetables. Get enough vitamin D through natural light and supplements, as this helps your body absorb calcium.
- Do regular exercise – doing three 30-minute weekly sessions of ‘weight bearing’ exercise has been shown to increase bone strength.
- Incorporate exercises such as brisk walking, modified weight training, dancing, jogging and aerobics into your daily routine.
- If you already have bone loss, avoid high impact exercises that can carry a high risk of falls or bone fracture. Exercises such as yoga, tai chi, swimming and water aerobics can help improve balance, core strength, flexibility and toning without causing further damage to bones. Talk to your healthcare team for advice.
- Hormone replacement therapy (HRT) – if you have reduced hormone levels, HRT may be beneficial as this is also an effective way to slow bone loss. This should be done after careful consideration and in consultation with your BMT team and endocrinologist.
Where can I find further information?
- Jean Hailes. Bone health. jeanhailes.org.au
- Healthy Bones Australia. healthybonesaustralia.org.au
- Musculoskeletal Australia. Understanding osteoporosis. msk.org.au