Back and Neck injuries
Back
Neck
Spinal Cord Injury
Back to the top
- “Spinal shock” – [NOT to be confused with neurogenic shock] is a transient state used to describe dysfunction of neurones following spinal ‘concussion’ (i.e. there is no demonstrable injury to spinal cord on MRI). Occurs within a few minutes of injury and lasts days to weeks but is associated with a good prognosis and potential for full recovery. It refers to a flaccid areflexia, rather than the loss of sympathetic vascular tone which accompanies neurogenic shock. Spinal shock and neurogenic shock may occur together, however, the terms have different pathophysiology and should not be used interchangeably.
- Hypotension and spinal injury. In the trauma scenario, a hypotensive patient is presumed to be HYPOVOLAEMIC until proven otherwise. Whilst other forms of shock must be considered in the background (e.g. neurogenic), always remember that hypotension + trauma = hypovolaemia, even IF your patient has a concurrent spinal cord injury.
- Consider the four levels and degree of spinal injury:
- Neurological level
- Sensory level
- Motor level
- Skeletal level
- Degree – complete or incomplete?
Cervical Spine Injuries
Back to the top
Initial Approach
- The mechanism of injury is essential to establish. Ask yourself, are there ‘high risk’** features to the presentation?
- Consider from the outset – are there features to the patient/ history that require mandatory radiology or make clinical clearance impossible?
- DOCUMENT, DOCUMENT, DOCUMENT. If a spinal injury is suspected, you should perform a thorough neurological examination, including a detailed sensory exam (if patient able to comply), log roll and rectal examination and document your findings carefully. This may occur prior to radiology. Your findings may have important implications for management, transfer, medico-legal sequalae and patient prognosis.
- The goals of initial emergency care for cervical spine injuries are to 1) resuscitate and haemodynamically stabilise the patient and 2) prevent secondary or further spinal injury
** axial load, fall >3m, MVA >60mk/hr, ejection from vehicle, vehicle roll over, neurological symptoms, distracting injury, significant con-currant or multi-system injuries, age >65, pre-existing cervical neck conditions.
Epidemiology and Patterns of Injury
- Male: female ratio 4:1.
- Two peaks of injury – young adults and those >65 years.
- Falls >2m and MVA most common causes.
- Remember the ‘3 column model’ – stability requires that 2 of the 3 ‘columns’ of the cervical spine remain ‘in-intact’. This will delineate stable vs unstable injuries.
- C2 most commonly fractured vertebra.
- C5-6 or C6-7 most common dislocations.
- Spinal cord syndromes.
Radiology
- Plain films will obtain an inadequate view in up to 35% patients, even with swimmers views.
- Cervical spine CT now often replaces plain films. Should be first investigation of choice in patients >65 years, obese, where there is an indication for CT head, patient has significant pre-existing spinal pathology and some other considered situations.
- MRI is the investigation of choice for ligamentous injuries/ spinal cord injury or oedema, however it is not that sensitive for detecting certain types of fracture (e.g. Jefferson fracture, pedicle fracture).
Fracture Types
- Will not be covered extensively here
- Know that mechanism affects pattern of injury
- Flexion, rotation, extension and compression injuries will present with different patterns both clinically and radiologically.
Further References and Resources
- Radiology Assistant - Is an excellent, comprehensive over view of cervical spine injuries from the department of radiology and regional spinal cord injury centre, Thomas Jefferson University Hospital, Philadelphia.
If you find one spinal fracture…look for the second!
Thoracolumbar Injuries
Back to the top
- If there is thoracolumbar fracture in trauma, consider the possibility of concurrent intra-abdominal/solid organ injury.
- Thoracic vertebral fractures are frequently missed on plain x-rays (will detect only 75%).
- Wedge/compression fractures are common in osteoporosis and may occur spontaneously. Remember the elderly person with back pain – a much lower threshold for considering imaging.
- Consider the ‘columns’ when assessing if a fracture is stable vs unstable.
- If anterior margin is reduced by >50% and/or posterior ligament is injured – it may be a potentially unstable fracture requiring surgery. Generally advised to progress to CT imaging for further assessment if >30% collapse. Otherwise, most wedge fractures are managed conservatively with symptomatic treatment, but the elderly may require admission for mobility or pain management.
- Chance fractures (disruption involving all three spinal columns) may be missed on CT without bony (saggital) reconstructions. The ‘typical’ flexion injury that is associated with lap belt use or fall from height and has a high rate of concurrent intra-abdominal pathology.
Remember – if you find one spinal fracture – look for the second…
Spinal Cord Syndromes
Back to the top
| Name | Type of Mechanism | Findings on Exam | Prognosis |
|---|---|---|---|
| Complete transection | Trauma, infarction, tumour | Complete loss of motor and sensory function below level | Poor |
| Central Cord Syndrome | Hyper-extension injury More common in elderly | Incomplete paralysis (distally weaker than proximal, and arms weaker than legs) Proximal decrease in pain/ temp sensation Vibration and proprioception spared Bladder dysfunction | Usually good |
| Anterior Cord Syndrome | Flexion injury (e.g. diving) | Lateral and anterior spinothalamic tract signs present Proprioception spared | Poor |
| Nrpwm-Sequard Lesion | More common with penetrating injury (e.g. knife) | Ipsilateral paralysis Contralateral spinothalamic loss | Good prognosis (similar to stroke). Usually retain sphincter control. |
| Dorsal Column Syndrome | Very rare in isolation | No good data |
Clinical Decision Rules
Back to the top
There are several, validated clinical decision rules. The Canadian C-spine rule and NEXUS are the two most clinically utilised in Australia. These two clinical decision tools help you to decide who needs radiology to rule out a significant cervical spine injury.
Have a working understanding of both rules. Whichever rule you chose to apply, complete all the components of that rule.
If a patient passes either rule they can be cleared clinically without injury. Specifically, the NEXUS rule allows you to clear patients with a serious mechanism of injury if they are symptoms free, where as The Canadian rules do not. However, the Canadian rules allow you to clear a patient with neck pain if they have low risk features, where as the NEXUS rule does not.
Canadian Cervical Spine Rule (Canadian C-spine Rule)
- 8900 patients. 100% sensitive, 42.5% specific.
NEXUS (National Emergency X-Radiography Utilization Study)
- >34,000 patients. It only included a very small number of infants, so be careful about applying rules to the paediatric populations.
- Found to be 99% sensitive for detecting ANY injury, 99.6% specific for detecting ‘significant’ injury. However, in patients >65 years, sensitivity dropped to only 89% for clinically significant injury.
- 12.9% specific.
Maintaining Cervical Spine Precautions
Back to the top
In recent years there has been increasing discussion around the use of spinal immobilisation both pre and in hospital, in particular the use of the rigid cervical collar and the evidence behind it (1-6).
There is no scientific evidence that any type of cervical collar used in prehospital transport or initial trauma management is effective in stabilising an acutely injured cervical spine or preventing further neurological deterioration in those with spinal cord injury (7). However, there is evidence that rigid collars can lead to significant complications and morbidity when used to secure the c-spine.
These complications include (11-13):
- Pressure areas of the scalp and neck
- Increased pain adversely affecting compliance with immobilisation strategies designed to protect patients from further harm
- Impaired jugular venous return and rises in intracranial pressure both in head-injured and healthy people
- Impaired respiratory effort and forced expiratory volume, particularly in older patients with chest injury or comorbid respiratory conditions, predisposing these patients to aspiration
- Increased complexity of airway management
- Increased extrication time and delay to definitive treatment
Evidence indicates that we are unable to completely immobilise the C spine in any collar and there is no data to support that any additional movement of an injured C spine causes more damage (13, 14).
After consultation with specialist clinicians across NSW and consideration of the available evidence, The Institute of Trauma and Injury Management (ITIM) and ECI have concluded that the risks of immobilisation with rigid collars outweigh the chance of benefit.
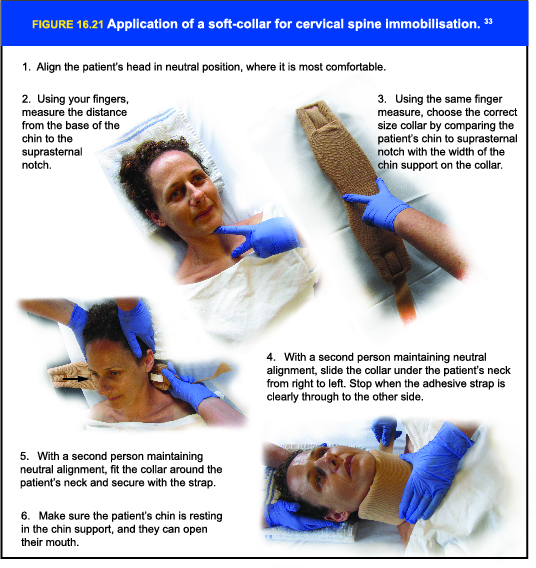
ITIM and ECI are advocating for the adoption of foam cervical collars in the initial management of injured adults and children requiring cervical spine precautions being transported by NSW Ambulance and presenting to NSW Health facilities.
For more information, please read our Position Statement on maintaining cervical spine precautions. This statement also covers application of foam collars in a variety of clinical scenarios.
Autonomic Dysreflexia
Autonomic dysreflexia is a medical emergency that can occur in people with spinal cord injury at or above the sixth thoracic (T6) level. It is a sudden and severe rise in blood pressure resulting from overactivity of an isolated sympathetic nervous system below the lesion, triggered by a nociceptive stimulus that can result in intracranial haemorrhage, fits, arrhythmias, hypertensive encephalopathy and even death. This potentially life-threatening condition requires immediate and decisive action. Below are some useful links to assist in the management of this condition in the emergency department:
Autonomic Dysreflexia Medical Emergency Card
Autonomic Dysreflexia Algorithm
Video Presentation on Autonomic Dysreflexia by Dr James Middleton
Safety Notice 14/10 - Autonomic Dysreflexia (revised) 2010
Management of the Neurogenic Bladder for Adults with Spinal Cord Injuries
Management of the Neurogenic Bowel for Adults with Spinal Cord Injuries
References and further resources
Back to the top
- Spinal Cord Injury Resources, Spinal Cord Injury Network, Agency for Clinical Innovation (ACI)
- Canadian C-Spine rule - Stiell et al, Ottawa Health Research Institute, Canada, 2003