Pelvic Inflammatory Disease - PID
Pelvic Inflammatory Disease (PID) is a syndrome comprising a spectrum of inflammatory disorders of the upper female genital tract, including any combination of endometritis, salpingitis, tubo-ovarian abscess and pelvic peritonitis. Arises from ascension of organisms from the endocervix, and is primarily sexually transmitted. Frequently there is no cause identified. However the most common organisms found are ascending vaginal organisms - gonorrhoea, chlamydia and mycoplasma.
Fitz-Hugh-Curtis syndrome is a complication of PID: it is characterised by inflammation of the membrane lining the stomach (peritoneum) and the tissues surrounding the liver (perihepatitis). Common symptoms include severe pain in the right upper quadrant of the abdomen, fever, chills, headaches and malaise.
Overview flowcharts
An overview flowchart is available here.
A table of common causes of low abdominal pain in women of reproductive age is available here.
History
Risk factors
- Early coitarche, high number of partners, age 15-25 years, unprotected sex.
- Recent insertion of IUD.
- Operative procedures - TOP.
- Post-partum infection.
- Rarely, descending infection from pelvis/abdominal cavity.
- Symptoms: abdominal pain, pelvic pain with sex, abnormal bleeding (“spotting” or irregular menses, post coital bleeding, change in vaginal discharge, urinary symptoms.
- Signs: one or more of cervical motion, uterine or adnexal tenderness +/- fever, cervicitis, adnexal swelling.
- Differential diagnoses: ectopic pregnancy, torsion or haemorrhage of ovarian cyst/tumour, threatened abortion/ retained products conception, urinary tract infection, appendicitis, endometriosis, Mittelsmertz, dysmenorrhoea.
Sexual history
Include sexual, menstrual, gynaecological and contraceptive history.
Sexual history should include:
- whether they have a regular partner and for how long
- when was the last time they had sex
- condom use
- when was the last time they had a different partner
Obtaining a reliable sexual history and disclosure requires using a sensitive approach and ensuring privacy which may not be easy to achieve in an emergency setting particularly among adolescent women.
Ultrasound
Ultrasound is the preferred examination for young women with lower abdominal pain as it does not involve radiation. Transvaginal ultrasound (TVUS) is recommended except in young women who are not yet sexually active. TVUS is best in urgent cases e.g. ectopic/ovarian torsion and can be performed without the need for a full bladder.
The indications for TVUS in young women with lower abdominal pain are:
1. When pregnancy test is positive - to assess for ectopic pregnancy.
2. When severe pain/peritonism is present - TVUS can reduce the negative appendicectomy rate by identifying women with gynaecological causes of pain.
3. When a pelvic mass is felt on bimanual examination - TVUS should be performed to help diagnose the mass.
4. Failure to respond to initial management for PID or if diagnosis is unclear - to assess for other diagnoses.
Findings
Ultrasound is useful for visualisation of the ovaries and is usually able to identify ovarian cyst complications. Note that small ovarian cysts may be present, without being the cause of pain.
A normal ultrasound or small amount of fluid in the pouch of Douglas may be consistent with appendicitis or PID. If the appendix is visualised it can assist in the diagnosis of appendicitis.
Features that may be consistent with PID are:
1. Normal ultrasound
2. Fluid in the pouch of Douglas
3. Thickening or increased vascularity of the fallopian tubes
4. The presence of a tubo-ovarian abscess.
Investigations
1. Pregnancy test (Beta hCG on urine OR serum)
2. STI check
- Chlamydia and gonorrhoea PCR (swab OR urine*)
- Endo-cervical swab if speculum examination performed OR
- High vaginal swab# (practitioner OR self-collected) OR
- First pass urine* for chlamydia / gonorrhoea PCR if swabs unable to be taken (less sensitive)
- +/- Mycoplasma Genitalium PCR
- A second high vaginal swab or first catch urine should be sent for mycoplasma genitalium only if the decision is made to treat the patient for PID.
- High vaginal swab for M/C/S
#Self collection for high vaginal swab is an equal alternative to practitioner collection.
*First pass urine for chlamydia/gonorrhoea PCR if swabs unable to be taken.
3. Urinalysis*
- Send for M/C/S if WCC+/or nitrites detected and dysuria, frequency or renal angle pain are present.
*It is important that the specimen is a clean catch MSU due to risk of contamination in patients with potential PID and vaginal discharge.
4. Blood tests
- FBC, EUC
- Other tests to be ordered if appropriate clinical indications present e.g. LFTs / lipase in patients with referred RUQ.
- CRP is unlikely to be useful
Speculum and Bimanual Examination
A speculum and bimanual examination is important, as it will provide additional information that supports the diagnosis of PID. It can also be useful to rule out PID.
It may be reasonable to not perform this examination if:
- the patient refuses
- it is likely that the examination will need to be repeated by the O&G team
- the patient is a young woman who is not yet sexually active.
If speculum and bimanual are not performed, treatment for PID should still be commenced if:
1. the diagnosis of PID is highly likely based on history, risk factors and abdominal palpation,
OR
2. no other diagnosis is obvious. Improvement in symptoms after commencement of treatment provides supportive evidence for the diagnosis of PID.
Speculum examination
1. Note appearance of the cervix
Signs of cervicitis which support the diagnosis of PID are:
1. Mucopurulent discharge | 2. Prominent ectropion 3. Friability and easy bleeding |
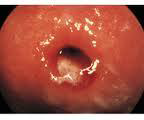 | 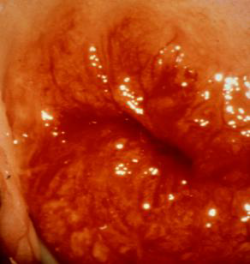 |
2. Take cervical swab for NAAT (PCR) for chlamydia and gonorrhoea
3. Collect a high vaginal swab for M/C/S
Bimanual examination
1. Check for tenderness. Any of the following support the diagnosis of PID:
- Cervical motion tenderness – an increase in pain when the cervix is rocked back and forth
- Uterine tenderness – tenderness felt when the uterus is felt between the examiners’ two hands
- Adnexal tenderness – tenderness felt when palpating lateral to the uterus
The absence of cervical motion, uterine or adnexal tenderness makes the diagnosis unlikely.
2. Check for masses within the pelvis.
It is common to be able to palpate the ovaries of young women.
In PID the adnexal tissues (fallopian tube and blood vessels) may feel swollen.
If any other mass is felt within the pelvis, arrange a TVUS.
Management
Treatment should be commenced without waiting for test results. Antibiotic treatment should be initiated in ED.
See therapeutic guidelines for up to date guidelines on antibiotic therapy.
Mild to moderate disease
Outpatient therapy | |
Preferred regimen | Alternative regimen*^ |
Ceftriaxone 500mg IM or IV stat Azithromycin 1g PO stat Metronidazole 400mg PO bd for 14 days# Doxycycline^ 100mg PO bd for 14 days | Ceftriaxone 500mg IM or IV stat Azithromycin 1g PO stat Metronidazole 400mg PO bd for 14 days# Azithromycin 1g PO single dose 1 week later |
*For patients who may be non-compliant to doxycycline, consider alternative regimen
^ If pregnant or breastfeeding, avoid doxycycline and use alternative regimen
# Tinidazole 2g stat is an alternative to metronidazole only where compliance is likely to be poor. Avoid in pregnancy and breastfeeding.
Severe
Consider admission for inpatient care and intravenous antibiotics for patients if:
- there is suspicion or definitive diagnosis of tubo-ovarian abscess
- systemically unwell
- no response to outpatient therapy
- pregnant
- diagnosis uncertain
Inpatient therapy |
Ceftriaxone 2g IV daily OR Cefotaxime 2g IV tds Azithromycin 500mg IV daily Metronidazole 500mg IV bd |
When discharged from hospital, patients should receive a supply of or prescription for antibiotics to complete oral outpatient therapy (as above).
Other management
- Patients to avoid sexual intercourse with regular partner until after one week following treatment
- Consider prophylactic treatment for Candida infection
- Provide patient with Factsheet
Contact tracing
Current sexual contacts should be treated with Azithromycin 1g PO stat, irrespective of test results.
Follow up
Patients should be advised to follow-up with their local Sexual Health clinic (or GP if preferred) within 2-3 days to assess for response to treatment.
Further References and Resources
- eTG: Therapeutic Guidelines - pelvic inflammatory disease