The living well in multipurpose services (MPSs) resources support staff to provide care for residents of these facilities. The aim is for people to be treated as though they are living in their homes rather than as patients in a hospital.
Key resources

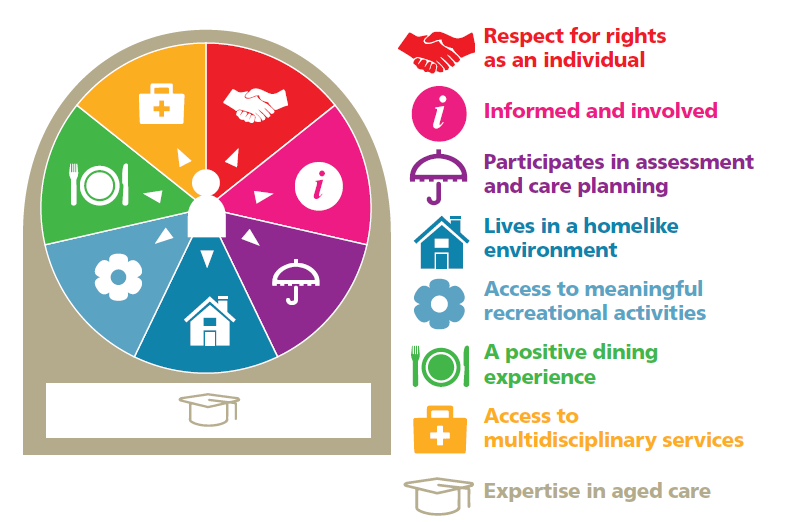
Principles of care
Published September 2016. Next review: 2024.
Improve the quality of life and wellbeing for residents.
Download the principles of care (PDF 966.5 KB)

Resource guide
Published September 2016. Next review: 2024.
Use these resources and strategies to improve your service.
Download the resource guide (PDF 984.2 KB)

Self-assessment
Published: August 2017. Next review: 2024.
Identify the strengths and weaknesses of your service.
Download the self-assessment tool (PDF 820.3 KB)
Supporting resources
- Backyard chickens (PDF 72 KB) – Use these guidelines to safely keep chickens in the backyards.
Source: HealthShare NSW. Published: September 2017. - Composting (PDF 44 KB) – Compare worm gardens and regular composting.
Source: HealthShare NSW. Published: September 2017. - Home grown produce (PDF 44 KB) – Safely grow, store and prepare produce.
Source: HealthShare NSW. Published: September 2017. - Food item brought in (DOC 49 KB) – Register food brought in by families and carers.
Source: HealthShare NSW. Published: January 2018. - MPS principles in practice: Summary (PDF 122 KB) – Support your case for change with the statistics and actions behind the principles.
Source: ACI. Published: April 2018. - Animal visits and interventions in public and private health services NSW (GL2012_007) – Use these guidelines for visits from pets, resident and therapy animals.
Source: NSW Ministry of Health. Published: September 2012. - Top 5 toolkit: residential aged care facilities (PDF 2.6 MB) – Work with carers to understand your residents
Source: Clinical Excellence Commission. Published June 2014. - This is me (PDF 244 KB) – Record the routine and preferences of your residents dementia, delirium or other communication difficulties.
Source: Alzheimer’s Society (UK). Published: March 2022.
Background
MPSs are unique healthcare facilities providing small rural communities with a combination of emergency, acute, community based and residential aged care services. There are 64 MPSs spread across NSW, providing hospital services for rural communities as well as a home for hundreds of older people.
The provision of a homelike environment; including lifestyle, leisure and activity options, nutrition and independence are crucial components contributing to wellness.
Outcomes
An evaluation in 2019 examined:
- the extent that the standards were implemented
- resident, carer, family and staff experience
- benefits to the healthcare system.
Results
- An average improvement of 20-40% across all eight principles of care.
- The principles with the greatest achievement were:
- recreation and leisure
- positive dining experience
- home like environment.
- Most MPSs integrated community activities with residential living to maintain connectivity and meaningful relationships. Examples include: school visits, BBQs, volunteer led outings, men’s sheds, raised vegetable gardens, chicken coups and restoring outdoor furniture.
- Widespread uptake of person-centred care has involved residents and families in case conferencing, care planning and decision making, based on lifestyle and individual daily routine and choices.
- Residents reported a marked improvement in relationships, independence and physical wellbeing. This reflects a cultural shift away from care based on clinical need to care based on lifestyle and enablement.
The principles of care are embedded as a resource in the National Safety and Quality Health Service Standards Aged care module and User Guide for Multi-Purpose Services.
More information
Additional resources, including an evaluation report, are available to network members via the network SharePoint site. Join the network or email ACI-Rural@health.nsw.gov.au
